With so many unnatural foods, including GMOs, in our diet these days, it seems as if digestive problems have become an epidemic in the United States. Dr. Matthew Marturano, a naturopathic digestion specialist, has seen it firsthand, and taken it upon himself to help fix this debilating and persistent problem that shows no signs of slowing down in the general population.
Scroll down toward the bottom of this article to see Dr. Marturano’s thoughts on colon cleansing and whether it’s really a good idea or not.
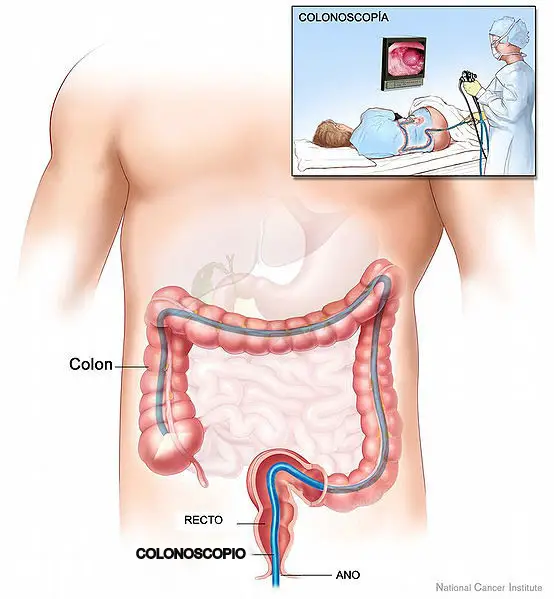
Are colon cleansings really worth it or are they worthless like mainstream doctors often say? Read on.
In this interview, Dr. Marturano spoke about what he’s seen as a holistic doctor on digestive health, his philosophy for helping to fix digestive issues in his patients and more:
AHW: Tell me a little bit about your title and credentials, also how you get started in the area of digestive health (and holistic health for that matter).
MM: I hold a Bachelor’s of Science in Biology and Philosophy from the University of Michigan, and a Doctorate in Naturopathic Medicine from the Southwest College of Naturopathic Medicine. The latter is a four-year medical program which combines training in conventional “Western” medicine, along with natural and alternative medicine, such as clinical nutrition, herbs and dietary supplements, mind/body medicine, and Traditional Chinese Medicine and acupuncture. I’ve also passed a national licensing board exam, and hold a license to practice naturopathic medicine from the State of Washington. Currently, my home state of Michigan does not have any licensing laws regulating naturopathic physicians.
While my training qualifies me to work with a wide range of conditions, when I got into practice I found that about 80% of the people who were coming to see me had digestive symptoms as their primary complaint. In addition to this, recent research has been drawing links between digestive health and other seemingly disparate conditions, such as autoimmune disorders, chronic inflammatory conditions, and mental/emotional challenges. Due to the overwhelming presentation of digestive disorders to my practice, along with the sheer volume of research that is being conducted in this area, I decided that focusing exclusively on digestive health would be the best way to serve my clients.
Buy organic superfood bars from Paleo Valley here
These are the best and most-nutrient dense nutrition bars on the market that I have found
AHW: What are the biggest digestive issues you’re seeing in patients and what is the general protocol for addressing them? Also, have you been seeing a rise in digestive issues lately?
MM: The majority of people that I see are dealing with some kind of functional digestive disorder, such as irritable bowel syndrome. The term “functional” is generally applied when there is some impairment of the ability of the digestive tract to perform its normal activities, however there are no structural abnormalities that can be detected by imaging studies or blood tests. Approximately 25% of Americans have some level of chronic functional digestive disorder, and an additional 55% complain of intermittent digestive disturbances. On top of these functional digestive disorders, many people are also presenting with multiple food sensitivities.
The incidence of functional digestive disorders appears to be on the rise, however as with many conditions, it is difficult to discern whether our observations are simply due to improvements in detection and reporting methods, or other factors. There appears to be some correlation between the increase of functional digestive disorders and the introduction of new and increasing amounts of chemical agents into the food supply. Concomitant with this is an increased consumption of highly processed foods, along with a reduction in the consumption of whole foods.
The protocol I am developing for dealing with functional digestive disorders is called The COHERENT Method. The word “COHERENT” is an acronym whereby each letter refers to one aspect of digestive function. For example, “C” stands for “Colonize” which refers to the introduction of beneficial microbes into the digestive ecosystem, which is often altered due to overuse of antibiotics. The methodology allows for a “COHERENT” overview of digestive function, while allowing for customized interventions unique to the individual. It incorporates nutrition, exercise, and lifestyle modifications along with dietary supplements and functional digestive lab testing, when appropriate. In my experience, I have found that “one size fits all” approaches to health conditions are unsatisfactory with respect to achieving positive and sustainable results.
AHW: What are maybe the three best additions to someone’s diet or lifestyle for fixing digestive issues, and the three things they can stop doing or remove from their lives or diets that will help the most?
MM: With respect to the diet, one of the first things I generally recommend is to increase consumption of cultured and fermented foods, which contain probiotic bacteria that have been shown to benefit digestive health. Adequate intake of dietary fiber is also a key element, as fiber helps to regulate gut motility, clean out debris, and also acts as a food substrate for gut microbes. However, in a fair number of people, these dietary modifications can result in a worsening of symptoms until other issues are addressed. Part of the goal of The COHERENT Method is to, not only learn what works, but to discern the correct order for introducing changes in a given person.
From a lifestyle perspective, a good place to start is to simply revisit one’s relationship with food. Due to our hectic lifestyles, food is often viewed as secondary to other “more important” activities, or in some cases even a nuisance. Re-learning to have a healthy relationship with food can go a long way to shifting how the body responds to it, once consumed.
In terms of things to stop doing, one of the first would be to stop eating and drinking things which cause one to feel poorly later on. It may seem obvious, but often times people aren’t making a clear connection between what they eat and how they feel. In the case of food sensitivities, there is often a significant delay (up to three days) between eating a particular food, and the development of symptoms. For other people, it often involves a reprogramming of our beliefs around punishment and reward which compel them to “reward” themselves with unhealthy foods, and to view eating healthy foods as a form of punishment or unwelcome restriction.
The kinds of foods I would recommend avoiding for people with digestive issues include wheat, corn, and dairy, as these are the three foods that people are most likely to be sensitive to. Very likely, this is simply due to the overconsumption of these foods in the average person’s diet. For most people, consumption of these foods in moderation is fine, however in some it is necessarily to remove one or more of these foods completely. Often times, after the gut has been rehabilitated, we can introduce foods back into the diet. However, in some situations, for example in Celiac disease, it may not be possible to reintroduce a food without an aggravation of symptoms.
AHW: What are the main differences between your approach and the “mainstream medical” way of thinking?
MM: Most medical interventions revolve around blocking a biochemical pathway (in the case of drugs) or removing diseased tissue (in the case of surgery). While these methodologies are often helpful, and sometimes necessary, they often lead to complications and side-effects in the long term that are deemed worse than the original condition. The work that I do is more focused upon supporting a biochemical pathway and the rehabilitation and healing of diseased tissue. Generally speaking, I believe the “supportive” approach to health seems most effective when applied early on in a disease process, rather than as a course of last resort. Another distinction I might draw is that natural medicine tends to be more proactive in its approach, while “mainstream medicine” is largely reactive.
However, there are no hard and fast lines between the two approaches. In my opinion, a full integration of both approaches would be the ideal setting for the effective practice of medicine. Unfortunately, many practitioners on either side of the fence seek to undermine the validity of those whom they perceive to be philosophical opponents. In the end, the practice of medicine means doing whatever demonstrably works, and good medicine means doing whatever works, while causing the minimum amount of harm or collateral damage.
AHW: A friend told me she has a “reasonable doctor” who said that colon cleansing is overrated…and that he’s “seen a lot of colons” that didn’t need to be cleansed and that the whole cleansing idea is not that important (editor’s note, I was just playing devil’s advocate on this question)…what are your thoughts on this?
MM: I think there is little doubt that colon cleansing is overrated, but that is not to say it is without value. Much of the practice hearkens back to a time when a particular theory of disease known as “autointoxication” was very popular. This theory hypothesized that disease was caused by a buildup of “toxins” within the gut which needed to be removed in order to restore health, for which frequent enemas and colon cleansing were regularly prescribed. While we now know that certain elements of the theory have some validity to them (for example, certain pathogenic bacteria in the gut can ‘deconjugate’ waste products secreted into the gut, which can lead to their reabsorption into the bloodstream), many of the proponents of autointoxication went too far in their claims, declaring that the process was responsible for nearly all disease, and therefore the removal of toxins, or detoxification, was the most appropriate strategy to improve health for everybody.
These superfood bars from Paleo Valley are rich in fiber
Try them today in flavors like red velvet, cacao-rich chocolate (On Sale Now)
One of the major shortcomings of this approach is the overemphasis on “eliminating the negative” in contrast to “accentuating the positive” which results in an endless stream of more and more austere diet and lifestyle practices in order to maintain health. While it is of course helpful to reduce the “toxic” burden on the body, it is important to realize that the body is well-suited to handling all manner of potentially harmful substances, and will do so given healthful amounts of clean water and air, sunlight, nutrition, as well as a good balance between activity and rest. In a nutritionally-depleted, or otherwise imbalanced internal and/or external environment, the body’s ability to maintain health despite a toxic burden can become severely impaired. In these types of situations, no amount of “cleansing” will result in the long-term restoration of health, and may make things worse. The effect is not dissimilar to what happens when chronic dieters experience that, with each new round of dieting, their bodies seem to put on excess weight easier than before.
That all being said, I do believe that colon cleansing can be of benefit when performed by a responsible practitioner in the context of a broader program that addresses the many other components of healthy digestive function. In my opinion, when a “cleanse” is the only thing offered and/or is being presented as a panacea, this raises some questions about the training and motivations of a given practitioner.
AHW: Thanks so much for joining us!
MM: Thanks for having me.
This article was first published in 2013 and updated in 4/24. For more articles like these in your inbox, click on this link.
Related Reading: America’s Favorite Protein Bar Has a Dirty Little Secret Most Haven’t Heard About Yet
Thanks for installing the Bottom of every post plugin by Corey Salzano. Contact me if you need custom WordPress plugins or website design.






